Introduction
Acute mesenteric ischemia (AMI) may be caused by a sudden decrease in blood flow to the intestine and cause intestinal infarction. AMI has a very low frequency of 1% to 2% of all abdominal emergencies, but a very high mortality rate of 50% to 70%. In particular, acute superior mesenteric artery embolism (ASMAE) accounts for about half of all AMI cases and causes sudden, very severe abdominal pain [1,2]. In practice, most patients are diagnosed with a very advanced stage of ASMAE due to its very rapid clinical progression.
Mesenteric angiography is known as a representative diagnostic method for identifying ASMAE [3], but mesenteric angiography is time-consuming, and has limited availability, consequently it is being replaced by computed tomography (CT) angiography [4].
Once the diagnosis for ASMAE has been confirmed, an emergency surgical exploration should be performed promptly to alleviate the ischemic bowel [5]. The exploratory laparotomy and surgical removal of the clot is the standard treatment method [6]. It is very important to reduce the operation time to prevent the progression of sepsis. However, for a non-vascular surgeon, the procedures of embolectomy, and the confirmation of reperfusion in the operating room may be a very difficult and time-consuming process. Thus, we report on a 68 year old male who underwent laparoscopic small bowel resection after percutaneous aspiration embolectomy for ASMAE.
Case Report
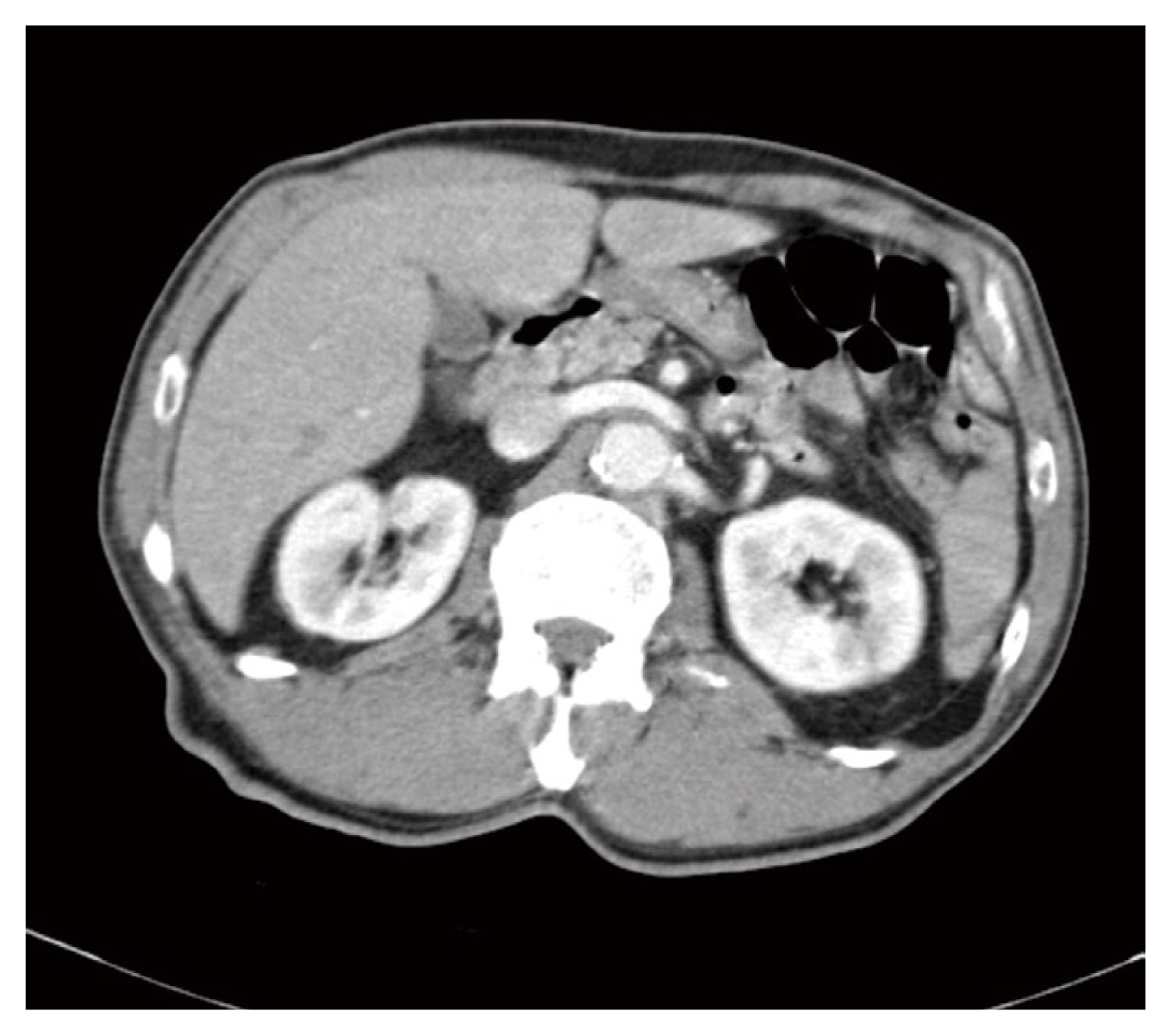
A 68-year-old man was referred to the Hanyang University Guri hospital for management of pancreatitis. He had epigastric pain and vomiting 6 hours previously. He had a history of chronic obstructive pulmonary disease, heart disease, and diabetes. He was a current smoker and had a history of smoking at least 40 packs per year. In a computed tomography scan previously performed at another hospital, there were no other findings other than several small infarctions of the spleen (Figure 1). He was hospitalized upon arrival at Hanyang University Guri hospital, an electrocardiogram and cardiac biomarker Tropin I was performed. An emergency coronary angiography was performed because a V4ŌĆō6 ST segment depression was observed on the electrocardiogram, and the level of troponin I was 0.049 ng/mL (normal range in Korea 0ŌĆō0.029 ng/mL). However, an angiography showed he had normal coronary arteries. A subsequent transthoracic echocardiogram showed no abnormalities except for apical hypertrophic cardiomyopathy. The patient complained of severe abdominal pain after angiography and echocardiography.
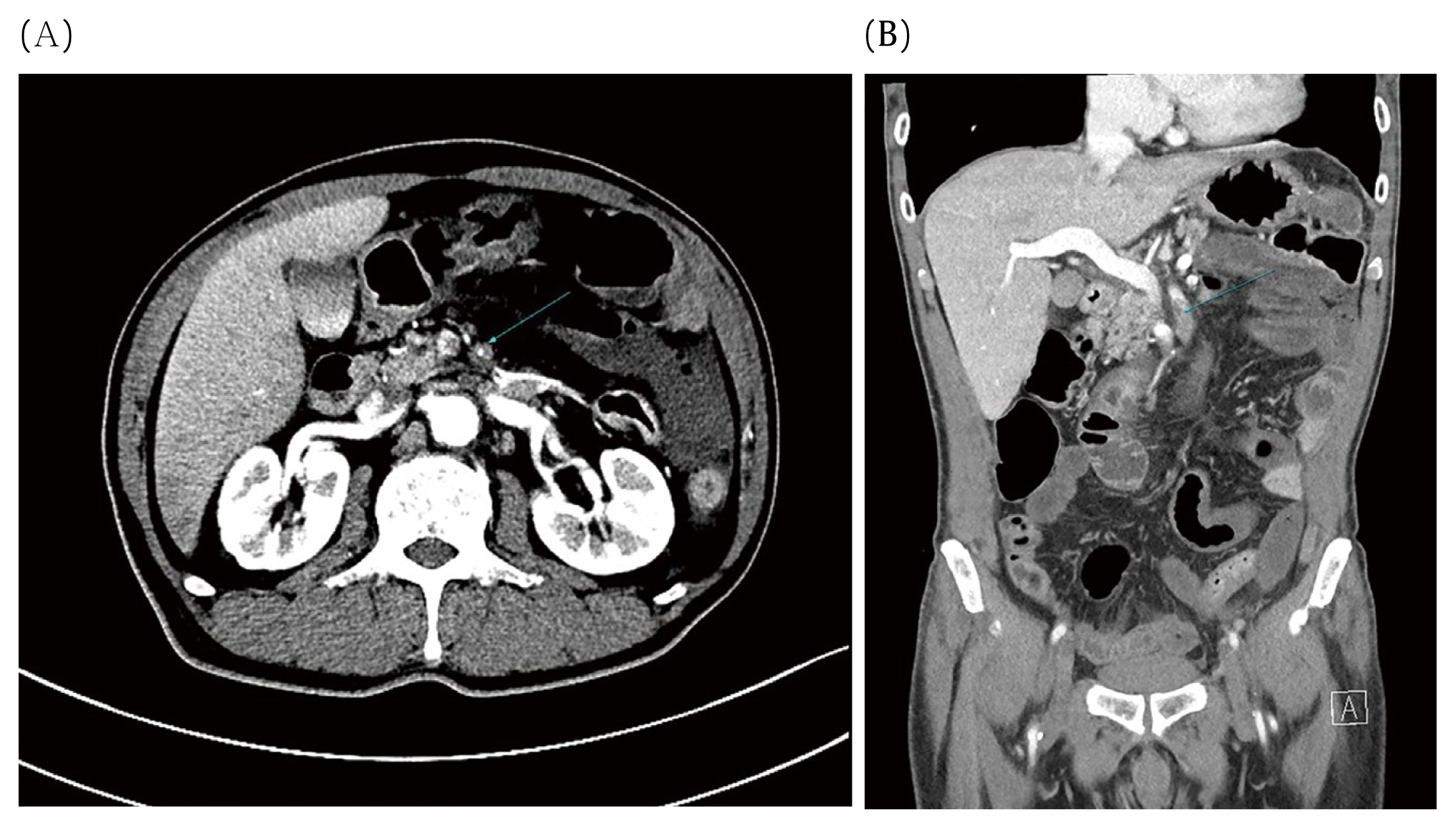
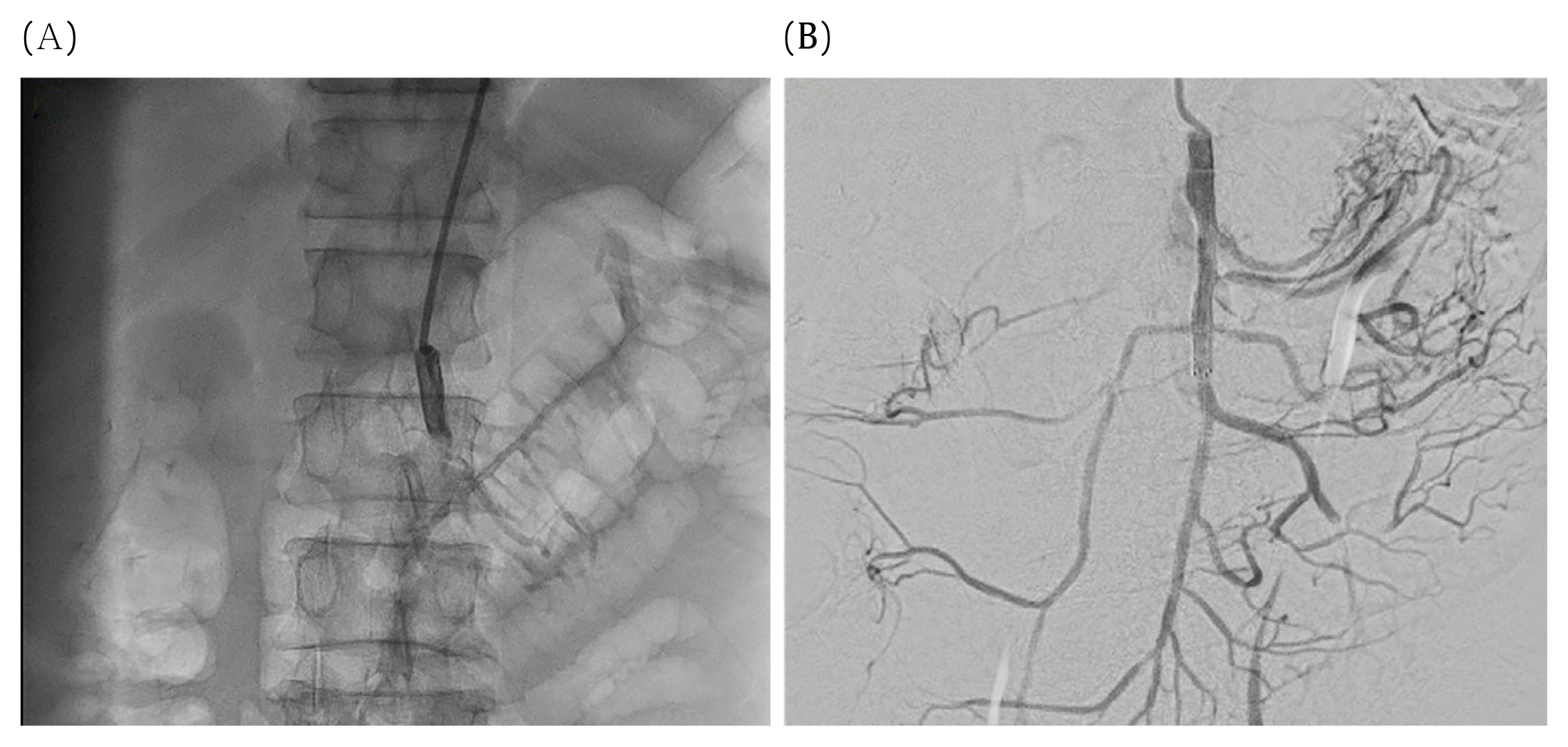
An urgent surgical consultation was performed to distinguish whether the peritonitis required surgical treatment. The abdominal CT with angiography showed occlusion of the superior mesenteric artery caused by an embolism (Figures 2A and 2B). An abdominal radiologist determined there was ischemic change of the whole of the small bowel. It took a total of 20 hours from hospitalization to diagnosis. The patientŌĆÖs hemodynamic signs were stable therefore, interventional vascular exploration was prioritized rather than a surgical approach. Percutaneous aspiration embolectomy was performed by an experienced cardiologist. After the embolectomy, there was no residual emboli in the jejunal and ileal branch (Figure 3). The white blood cell count was 22,300 per ╬╝L of blood before the procedure and dropped to 12,300 per ╬╝L of blood after the procedure. Given the effect of the embolectomy, surgical observation was performed for 10 hours to observe potential signs of ischemic bowel to determine the outcome of bowel resection, and ensure that the extent of small bowel necrosis was kept to a minimum.
During surgical observation, the patientŌĆÖs pain became more severe and the decision was made to perform emergency laparoscopic surgery. His American Society of Anesthesiologist score was graded as 3E because he was a heavy smoker and had lung disease. His body mass index was 19.6 kg/m2 (height 172 cm, weight 58 kg).
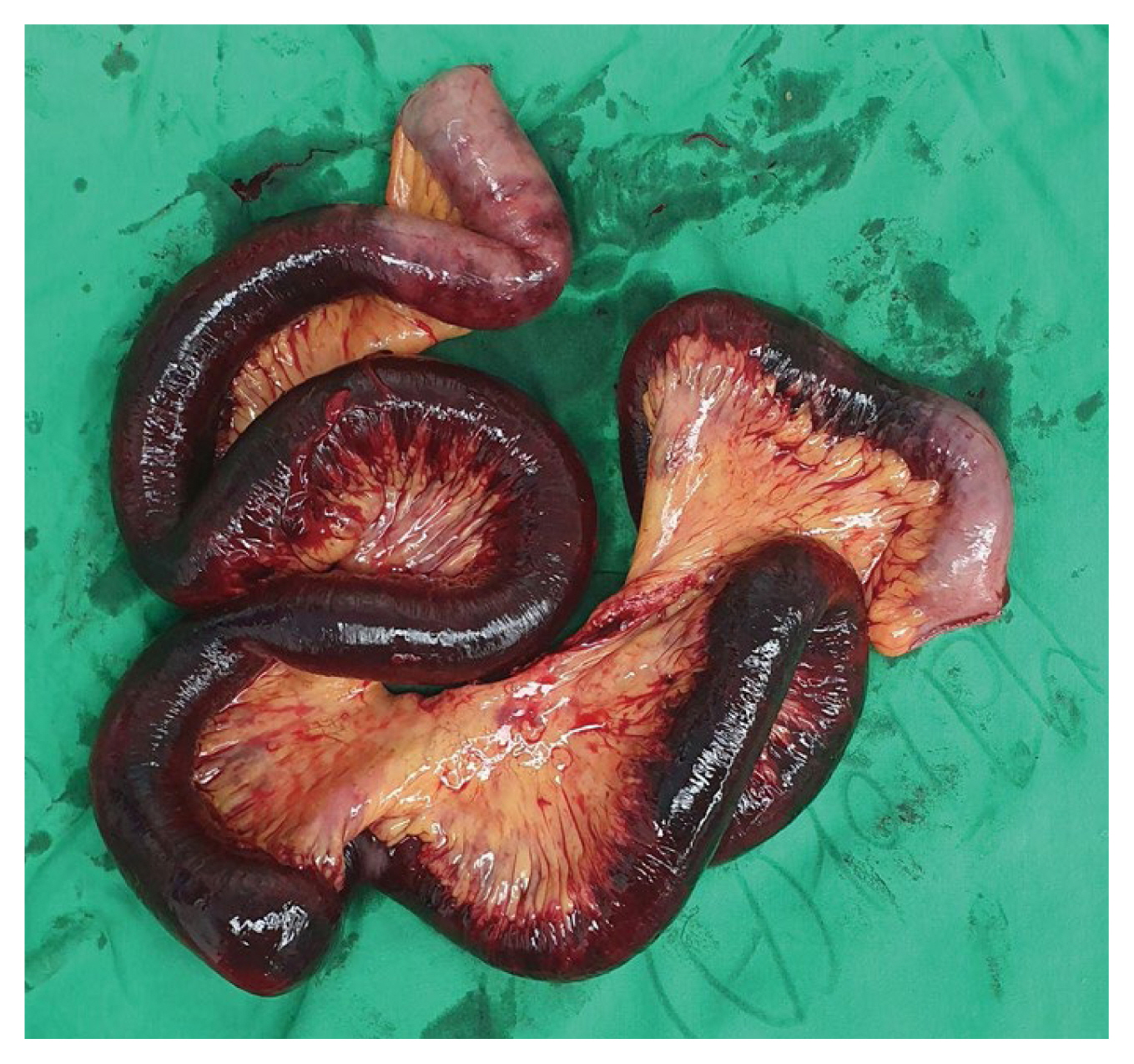
Laparoscopic surgery was determined as the surgical method of choice because there was no abdominal distension or clinical evidence of septic shock. In addition, laparoscopic surgery was chosen because a second operation may be necessary if the state of the bowel ischemia or infarction was difficult to confirm. The patient was placed in the reverse Trendelenburg position. After the initial trocar had been placed, the whole intestine was observed in the order of stomach, small intestine, and colon. The small bowel necrosis began 1.3 m below the Treitz ligament, and ended 30 cm above the ileocecal valve. The umbilical port incision was extended 4 cm to 5 cm to allow confirmation of bowel viability. Small bowel resections were performed preferentially by using laparoscopic linear staplers (ECHELON FLEX ENDOPATH Stapler 60; Figure 4). Then, the side-to-side anastomosis of small bowel was performed by using laparoscopic linear staplers. The 50 cc of estimated blood loss was calculated by an anesthesiologist. The operation time was 55 minutes (from skin incision to skin closure).
Considering the possibility of additional bowel infarction due to aggravation of bowel ischemia, the patient was moved to the intensive care unit for surgical observation. During the 3 days in the intensive care unit, he did not require a ventilator or vasoactive drugs. The patient was moved to the general ward on the third postoperative day. His diet progressed to a liquid diet on postoperative Day 5 and to a soft food diet on postoperative Day 6. A cardiology consultation was performed due to arrythmia during the hospital stay. He was diagnosed with atrial fibrillation and was prescribed amiodarone, edoxaban, and clopidogrel. He was discharged from hospital on the 13th postoperative day. There was no postoperative complications during the recovery period, and 6 months after surgery, the patient was doing well without weight loss, hypoalbuminemia, or bowel habit change.
Discussion
Despite the progress of surgical and interventional techniques, outcomes of ASMAE patients are still known to be very poor because of diagnostic difficulties. According to one study, the survival rate is very low if the diagnosis of ASMAE is delayed over more than 24 hours after the onset of symptoms [7]. Although the diagnosis was delayed due to normal CT findings determined prior to his admission to this hospital, ASMAE was diagnosed quickly using the rapid cycle of CT scans and acted upon immediately by the surgeon. In addition, examinations including coronary angiography permitted rapid exclusion of cardiovascular disease.
Therefore, if a patient has symptoms of peritonitis, active participation of a surgeon is necessary in the early stages of ASMAE. In particular, physicians should not hesitate to perform repeat CT scans due to the fear of using contrast agents.
In the treatment of ASMAE, early revascularization and reassessment of bowel are very important factors to improve surgical outcomes [8]. Traditionally, open surgery including embolectomy, endarterectomy, and bypass grafting have been associated with typical surgical methods [4]. However, most of the patients who undergo surgery for ASMAE are elderly patients with multiple comorbidities, and so non-invasive interventional procedures have been increasingly selected over the decades [9,10]. In general, interventional procedures can be attempted in the early stages of ASMAE. If there is any sign of suspected bowel necrosis, emergency open surgery is recommended.
A laparotomy is the best treatment method for ASMAE patients with suspected bowel necrosis. Surgeons should try to avoid the occurrence of short bowel syndrome by reducing the extent of bowel resection. During the operation, vascular procedures including embolectomy or endarterectomy can be performed to reperfuse the occluded artery. The bowel resection should be performed in the areas of necrosis to prevent sepsis progression. Bowel resection of the areas where necrosis is unclear must be withheld to prevent short bowel syndrome. A further operation can be planned to confirm the viability of the ischemic bowel.
However, in clinical practice, non-vascular surgeons have to spend a long time on vascular procedures. In particular, the long operation time can become a factor that results in a rapid deterioration of sepsis in elderly patients with multiple comorbidities. Therefore, the best method of surgery should be considered, alongside the hospitalŌĆÖs resources. A percutaneous aspiration embolectomy was performed prior to surgery. The patient was monitored constantly for 10 hours for signs of ischemic bowel to determine the outcome of the bowel resection. Due to the previous percutaneous aspiration embolectomy only bowel resection could be performed during the operation (the process of vascular exploration was not possible). The surgeon specialized in laparoscopic surgery checked the entire intestine and resected the area of bowel necrosis using laparoscopic methods. The operation time was less than 1 hour. The patient showed rapid recovery and was able to proceed with the a soft food diet 6 days after surgery.
We believe that the surgeon should participate in the team management of AMI. After the rapid diagnosis of the AMI, the patientŌĆÖs hemodynamic status and the hospitalŌĆÖs medical resources should be considered to establish the best treatment strategy. An interventional vascular procedure and consecutive laparoscopic surgery could be a treatment method.